The liver serves a multitude of vital functions crucial for the body’s well-being. Primarily, it aids in digestion by producing bile that assists in breaking down fats and certain vitamins. Additionally, it acts as a hub for nutrient processing and distribution throughout the body.
This powerhouse organ not only generates blood proteins and bile but also stores energy, fights infections, eliminates harmful substances from the bloodstream, and plays a pivotal role in metabolizing nutrients. Through its production of bile, the liver facilitates the breakdown of fats and aids in nutrient absorption in the small intestine. Once absorbed, various nutrients like sugars, amino acids, and vitamins travel via the bloodstream to the liver, which stores, processes, and distributes these essential elements as needed by the body.
Moreover, liver health encompasses a range of functions, including toxin removal from the blood, bile production, metabolism of macronutrients, regulation of blood cell volume, and synthesis of clotting factors. Glucose regulation is another crucial aspect; the liver manages blood sugar levels by storing glucose as glycogen and converting it back to glucose when the body requires more energy. It also converts other sugars into glucose, serving as a critical metabolic regulator.
Furthermore, the liver has a significant role in processing excess energy by converting carbohydrates into fatty acids or creating ketone bodies from fatty acids during periods of low carbohydrate intake or starvation.
Beyond energy metabolism, the liver synthesizes an array of essential molecules like albumin, cholesterol, uric acid, and various proteins involved in inflammatory responses and growth factors. Additionally, it plays a pivotal role in detoxifying harmful substances, transforming them into safer forms for elimination from the body. These substances include pharmaceutical drugs, environmental toxins, alcohol, and other compounds that could potentially harm the system if allowed to accumulate.
While the liver is naturally equipped to handle detoxification, some nutritional support is necessary for optimal functioning. However, the efficacy of many purported “detox” supplements lacks substantial scientific backing.
The liver also serves as a storage hub for numerous vital nutrients like vitamin A, copper, and vitamin B12, releasing them into the body as required. Its intricate involvement in storing, transporting, detoxifying, and synthesizing various substances underscores its integral connection to overall bodily health.
Despite its resilience, the liver can succumb to various diseases, some influenced by diet and lifestyle. Conditions like nonalcoholic fatty liver disease (NAFLD), including its advanced forms like nonalcoholic steatohepatitis (NASH) and cirrhosis, are particularly prevalent and merit attention due to their widespread impact on health. NAFLD alone affects a significant portion of adults in the US and Europe, emphasizing the importance of understanding and addressing liver-related concerns stemming from lifestyle and dietary factors.

Milk thistle
Milk thistle (Silybum marianum L.) contains silymarin, a mixture of plant compounds known to benefit injured livers.
Milk thistle has been used for centuries as an herbal remedy for liver disorders. Silymarin, which is a mixture of several different plant compounds known as flavonolignans, is the bioactive component, a complex mixture of plant-derived compounds identified as mostly flavonolignans, flavonoids (taxifolin, quercetin) and polyphenolic molecules.
Evidence suggests that silymarin protects liver cells, reduces liver-related deaths, and improves markers of liver function in people with chronic liver disease1. These effects are primarily attributed to silymarin’s role as a free radical scavenger, thus reducing oxidative stress and inflammation. Silymarin also seems to have antifibrotic properties.
Milk thistle extract and silymarin are best best-studied natural ingredients for liver health. They are constituents of drugs and food supplement products supporting liver health. Dosages of milk thistle extract and silymarin in those products depend on legislation in the market they are sold.
Silymarin acts as a free radical scavenger and modulates enzymes associated with the development of cellular damage, fibrosis and cirrhosis. These hepatoprotective effects were observed in clinical studies in patients with alcoholic or non-alcoholic fatty liver disease, including patients with cirrhosis. In a pooled analysis of trials in patients with cirrhosis, silymarin treatment was associated with a significant reduction in liver-related deaths. Moreover, in patients with diabetes and alcoholic cirrhosis, silymarin was also able to improve glycemic parameters. Patients with drug-induced liver injuries were also successfully treated with silymarin. Silymarin is generally very well tolerated, with a low incidence of adverse events and no treatment-related serious adverse events or deaths reported in clinical trials. For maximum benefit, treatment with silymarin should be initiated as early as possible in patients with fatty liver disease and other distinct liver disease manifestations such as acute liver failure, when the regenerative potential of the liver is still high and when removal of oxidative stress, the cause of cytotoxicity, can achieve the best results.
Silymarin: source and physicochemical properties
Silymarin consists of several flavonoid-like compounds extracted from the small hard fruits of Silybum marianum L. Gaertn (milk thistle), which grows extensively in Europe and Asia, including India. The drug belongs to a class of compounds—flavonolignans—likely produced in the plant by radical coupling of flavonoids and coniferyl alcohol. A reference composition comprises: silybin or silibinin (33.4%), silychristin (12.9%), silydianin (3.5%) and isosilybin (8.35%), which are assumed to be responsible for the therapeutic liver-protecting activity of the plant extract. The silymarin composition and the ratios of individual constituents may vary concerning different brands of commercial standardized milk thistle extracts. For the main component silybin, a large amount of pharmaco-toxicological and clinical documentation exists.
Although clinical trials have shown silymarin is safe at high doses (>1500 mg/day) in humans, the pharmacokinetic studies over the past three decades related to absorption, distribution, metabolism, and excretion of silymarin have revealed poor absorption, rapid metabolism, and ultimately poor oral bioavailability. For optimum silymarin bioavailability, issues of solubility, permeability, metabolism, and excretion must be addressed. An array of methods has been described in recent years that can improve its bioavailability, including complexation with β-cyclodextrins, solid dispersion method, formation of microparticles and nanoparticles, self-micro emulsifying drug delivery systems, micelles, liposomes, and phytosomes2.
Although the best-known and most studied natural ingredient connected to liver health, there are some limiting factors such as low solubility in water (<50 μg/mL), low bioavailability and poor intestinal absorption. To improve its bioavailability and provide a prolonged silymarin release at the site of absorption, the use of nanotechnological strategies appears to be a promising method to potentiate the therapeutic action and promote sustained release of the active herbal extract.
Figure 1 illustrates the types of formulations that have been developed to improve the solubility and bioavailability of silymarin, most of which being designed primarily for oral administration.
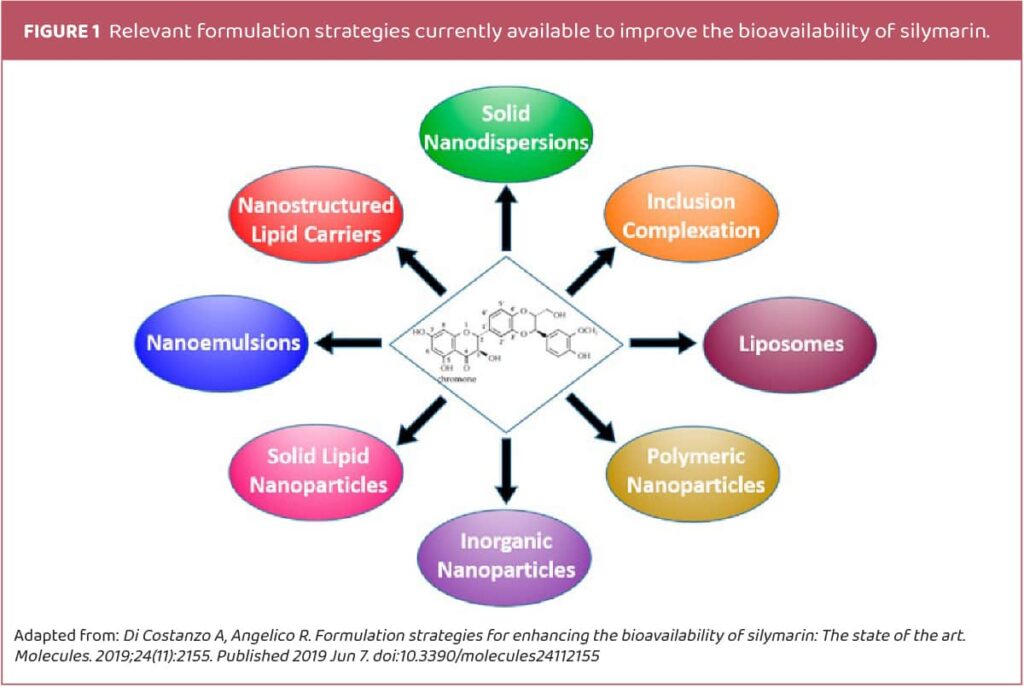
The therapeutic efficiency of silybin is rather limited by its very low water solubility. Another limiting factor consists of low intestinal permeability, which combined with poor water solubility, can cause lower efficacy.
Consequently, the product is poorly absorbed (20–50%) from the GIT and has a low bioavailability from oral formulations. So, continuous work on ways and strategies to overcome this is a crucial factor in the advancement of Milk thistle extract usage in oral dosage forms.
Artichoke extract
Artichoke extract is an extract from the common bulb vegetable (Cynara scolymus L.) that appears to have the ability to stimulate bile secretion; this may underlie a weak reduction in cholesterol and improved fat digestion.
It is grown in countries in the Mediterranean region, and has a high concentration of natural antioxidants such as mono-caffeoylquinic acid and dicaffeoylquinic acid (cynarin and chlorogenic acid), caffeic acid, and the volatile sesquiterpine and flavonoids and it also has an antimicrobial and cholesterol decreasing effects. Artichoke can have protective effects against NAFLD by reducing the production of reactive oxygen species, lipid peroxidation, and protein oxidation and increasing the activity of glutathione peroxidase.
A systematic review and meta-analysis were conducted to summarise studies conducted on the effects of artichoke supplementation on liver enzymes. Pooled analysis, of eight clinical trials, revealed that artichoke supplementation significantly reduced the concentration of aspartate aminotransferase (AST) and alanine transaminase (ALT), in comparison with a placebo. Subgroup analysis suggested that artichoke administration significantly reduces AST and ALT in patients with non-alcoholic fatty liver disease AST and ALT), and ALT among overweight/obese subjects.
Conclusions was the supplementation elicited significant reductions in liver enzymes, especially among patients with non-alcoholic fatty liver disease.
The study was limited by insufficient data, preventing a thorough examination of how artichoke leaf extract affects the ratio between AST and ALT enzymes. This ratio is considered a more reliable indicator of liver disease compared to just their levels. Consequently, interpreting the conclusions of this paper should be approached cautiously due to this limitation in the analysis of the enzymes’ relative changes3.
Another systematic review and meta-analysis aimed to assess the effects of artichoke administration on the liver enzymes. Pooled analysis of seven randomized controlled trials (RCTs) suggested that the artichoke administration affects both alanine aminotransferase (ALT), and aspartate aminotransferase (AST). Greater effects on ALT were detected in trials that lasted ≤8 weeks. Also, greater effects on AST were detected in trials using > 500 mg artichoke. Overall, this meta-analysis demonstrated artichoke supplementation decreased ALT and AST. However, further large, high-quality clinical trials in different regions are needed to provide definite conclusion. These findings provide additional evidence for physicians and medical researchers on the efficacy of alternative treatments for hepatic patients4.
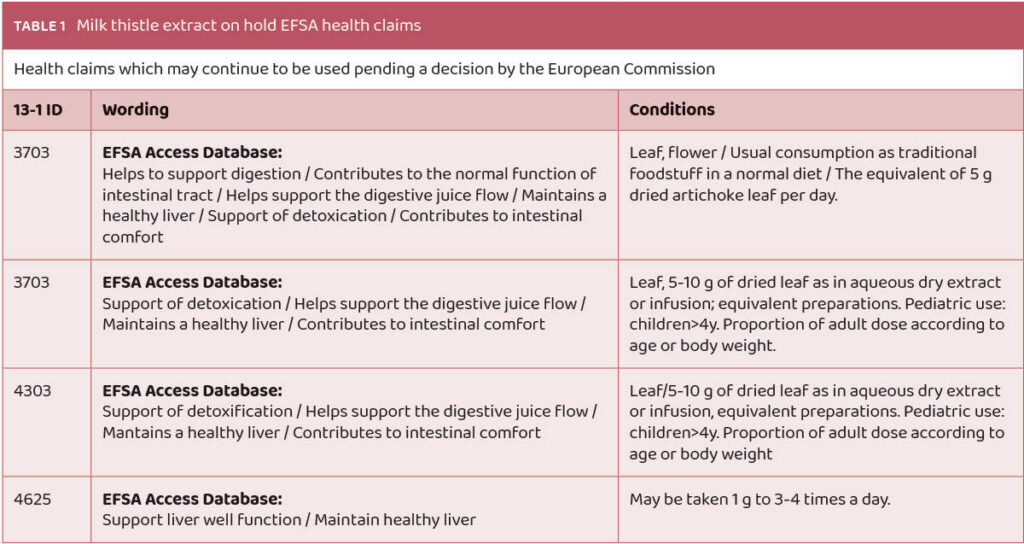
Artichoke extract has several on-hold claims pending connected to liver health. (Table 1)
Choline
Choline is crucial for various bodily functions: it’s a major component of cellular membranes and essential for neurotransmitter production, kidney function, and providing crucial components for various metabolic reactions. There’s a recommended intake, but actual consumption varies widely. The liver plays a key role in choline metabolism, crucial for methylation reactions, especially as it’s heavily involved in the process, affecting gene regulation and DNA methylation. Choline deficiency in the liver can impact mitochondrial function, leading to potential issues like inflammation, fibrosis, and even cancer development. This deficiency can influence epigenetic mechanisms, affecting how genes are expressed and impacting pathways involved in inflammation in the liver.
Dietary intake of choline varies over a three-fold range and many humans have genetic polymorphisms that increase their demand for choline. Choline is an important methyl donor needed for the generation of S-adenosylmethionine. Dietary choline intake is an important modifier of epigenetic marks on DNA and histones, and thereby modulates the gene expression in many of the pathways involved in liver function and dysfunction5. There is a recommended adequate intake for choline (about 550 mg/day), but choline intake in the diet has been estimated to vary by as much as three-fold – the lowest quartile and the highest quartile of intake were approximately 150mg and 500 mg/day choline equivalents.
Therefore, it is crucial to provide enough choline through supplementation, in case of lower or inadequate food intake for prevention of liver damage.
Vitamin E
Vitamin E encompasses a group of eight distinct compounds known for their antioxidant properties within the body. These compounds fall into two primary categories: tocopherols and tocotrienols, each further classified into alpha (α), beta (β), gamma (γ), and delta (δ) vitamers. While α-tocopherol is commonly regarded as the primary vitamer, research also focuses on the gamma variants (γ-tocopherol and γ-tocotrienol) due to their presence in the typical diet. Together, these compounds collectively constitute what is referred to as vitamin E. Notably, most vitamin E supplements predominantly feature α-tocopherol.
In one meta-analysis involving randomized controlled trials, the focus was on examining the impact of vitamin E supplementation on the blood levels of liver enzymes—specifically, alanine aminotransferase (ALT) and aspartate aminotransferase (AST)—in individuals diagnosed with nonalcoholic fatty liver disease (NAFLD) or nonalcoholic steatohepatitis (NASH).
A total of 794 individuals, comprising 470 adults and 324 children/adolescents diagnosed with NAFLD/NASH, were included in the analysis.
This analysis involved a review of 12 randomized controlled trials conducted across several countries, including the United States, Iran, Italy, Switzerland, Malaysia, Pakistan, and China. Among these trials, 8 focused on adults, while 4 targeted children/adolescents. In 7 of the trials, vitamin E supplementation was paired with lifestyle modifications in both the intervention and control groups. The dosage of vitamin E varied from approximately 150 to 900 IU per day, with placebos or no intervention used as comparators. The duration of the interventions ranged from 4 to 96 weeks.
The results demonstrated that compared to the control groups, supplementation with vitamin E led to a notable decrease in ALT levels by approximately 13.06 IU/L and AST levels by approximately 6.00 IU/L. Notably, these effects remained consistent across different population types (Asians vs. non-Asians) and age groups (adults vs. children/adolescents), varied intervention durations (≤24 weeks vs. >24 weeks), and whether lifestyle modifications were part of the intervention or not6.
Conclusion
The landscape of the food supplement industry has witnessed a notable shift in recent years, with an increasing emphasis on products tailored to support liver health. This surge in interest is propelled by several factors, collectively highlighting the pivotal role of the liver in maintaining overall well-being and the subsequent demand for supplements catering to its maintenance and enhancement.
One of the primary drivers behind this trend is the escalating prevalence of liver-related conditions, notably non-alcoholic fatty liver disease (NAFLD). Lifestyle factors, including sedentary habits and poor dietary choices, have contributed to a rise in these conditions. Consequently, there exists a burgeoning market for supplements purporting to fortify liver function and combat associated health issues.
The realm of athletic performance has also contributed to the propulsion of liver health supplements. Athletes, in their pursuit of peak performance and post-exercise recovery, seek supplements that aid metabolic processes, including those relevant to liver function.
There are not many new ingredients backed up with proven efficacy. Some relevant efficacy evidence exists for blends of a few herbs but as a standalone ingredient, silymarin is still the most studied and proven ingredient. This is due to the previously mentioned fact that it is present in products that are in the drug and also food supplements product category. As a drug compound, it had to be investigated thoroughly and to have proven efficacy. Other emerging ingredients and vitamins that are important for liver health are often still combined with silymarin.
While silymarin remains a well-studied and proven ingredient, the industry continues to explore novel concepts to fortify liver health, often combining emerging ingredients with established ones. This evolution presents opportunities and challenges for formulators and manufacturers, urging innovation and research to create advanced solutions that maximize liver health beyond existing supplements. As the pursuit of holistic well-being expands, the liver emerges as a key protagonist in the narrative of overall health and wellness.
References:
- Gillessen A, Schmidt HH. Silymarin as Supportive Treatment in Liver Diseases: A Narrative Review. Adv Ther. 2020;37(4):1279-1301. doi:10.1007/s12325-020-01251-y
- Di Costanzo A, Angelico R. Formulation Strategies for Enhancing the Bioavailability of Silymarin: The State of the Art. Molecules. 2019;24(11):2155. Published 2019 Jun 7. doi:10.3390/molecules24112155
- Moradi S, Shokri-Mashhadi N, Saraf-Bank S, et al. The effects of Cynara scolymus L. supplementation on liver enzymes: A systematic review and meta-analysis. Int J Clin Pract. 2021;75(11):e14726. doi:10.1111/ijcp.14726
- Amini MR, Sheikhhossein F, Talebyan A, Bazshahi E, Djafari F, Hekmatdoost A. Effects of Artichoke Supplementation on Liver Enzymes: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Clin Nutr Res. 2022;11(3):228-239. Published 2022 Jul 25. doi:10.7762/cnr.2022.11.3.228
- Mehedint MG, Zeisel SH. Choline’s role in maintaining liver function: new evidence for epigenetic mechanisms. Curr Opin Clin Nutr Metab Care. 2013;16(3):339-345. doi:10.1097/MCO.0b013e3283600d46
- Vogli S, Naska A, Marinos G, Kasdagli M-I, Orfanos P. The Effect of Vitamin E Supplementation on Serum Aminotransferases in Non-Alcoholic Fatty Liver Disease (NAFLD): A Systematic Review and Meta-Analysis. Nutrients. 2023; 15(17):3733. https://doi.org/10.3390/nu15173733




